Nocturnal hypoxia causes the activation of sympathetic activity through chemoreflex stimulation during apneic episodes. Sympathetic excitation may explain the association of nocturnal hypoxia with increased MEdif. Nocturnal hypoxia, characterized by severe oxygen desaturation, which is commonly observed in patients with obstructive sleep apnea, was associated with a hypoxia-peak SBP and nocturnal SBP surge and consequently may lead to increased morning BP. demonstrates that lower oxygen saturation (SpO 2) during the nighttime was associated with higher MEdif (≥20 mm Hg), independent of cardiovascular risk factors, among the outpatient population with at least one cardiovascular risk. Morning minus evening home BP (MEdif), calculated as the difference in the home morning BP and the evening BP, was significantly associated with a greater risk of CVD. Previous studies revealed that higher levels of HBPM were associated with an increased risk of cardiovascular disease (CVD), both in general and hypertensive populations. Home BP monitoring consists of performing morning and evening BP measurements twice on each occasion, with a minimum of 3 days and a preferred period of 7 days. In addition, HBPM is more practical in clinical practice than ABPM, particularly among those who are on antihypertensive medication. 
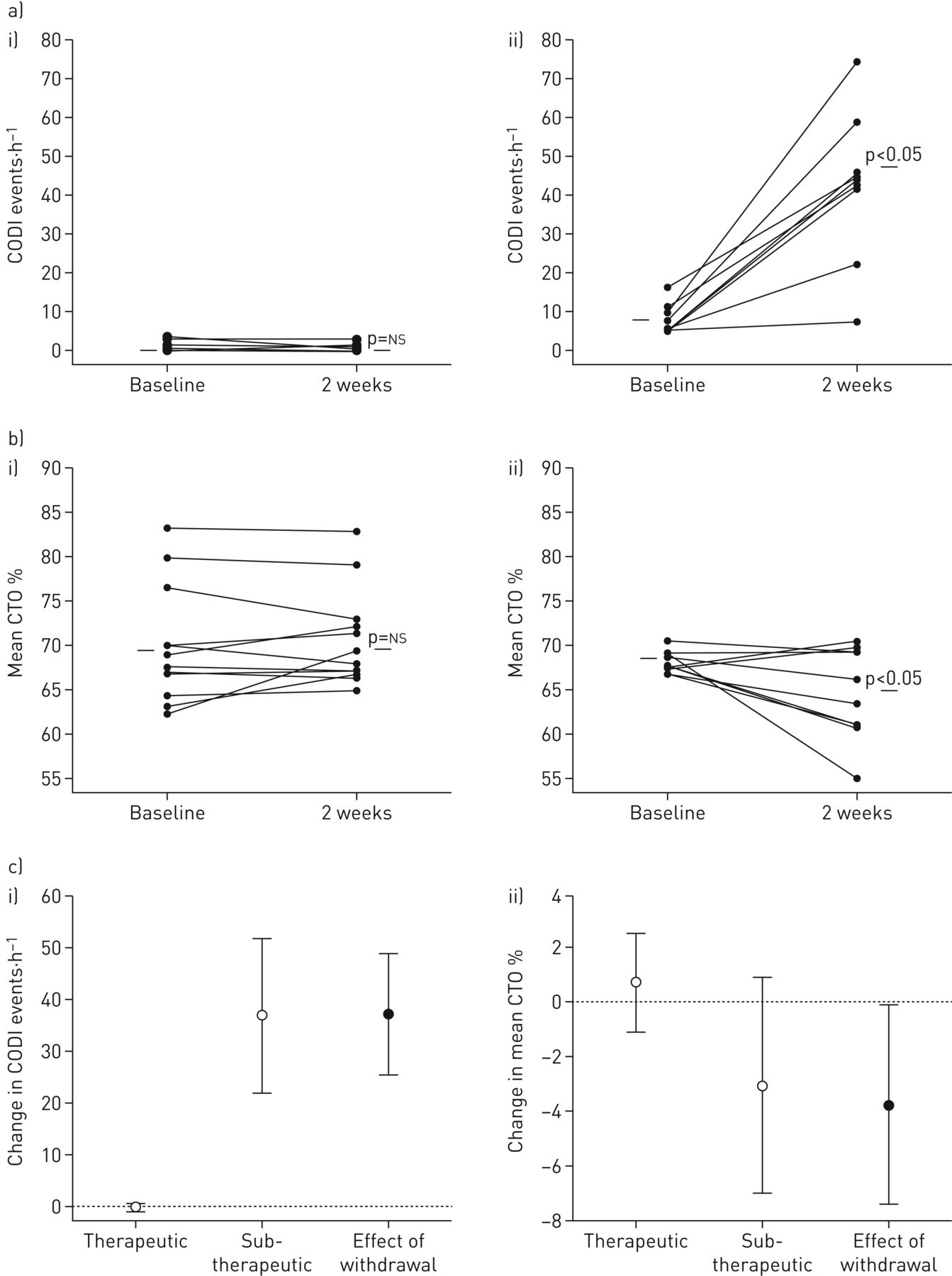
The prognostic value of home BP measurement (HBPM) is superior to that of office BP measurement and appears to be better than that of daytime systolic BP (SBP) and daytime diastolic BP (DBP) obtained from 24-h ambulatory BP measurement (ABPM). These validated approaches are able to identify hypertension phenotypes such as white coat hypertension and masked hypertension. Nocturnal hypoxemia Pulmonary arterial hypertension Sleep apnea.Globally, recent hypertension management guidelines have pointed out the importance of out-of-office blood pressure (BP), measured by home BP and 24-h ambulatory BP, for hypertension management. SA in patients with PAH was not associated with worse prognosis, unlike left ventricular heart failure, but nocturnal hypoxemia was related to poor prognosis. On the other hand, the mortality in patients with lower averaged SpO 2 was significantly higher than in those with higher averaged SpO 2 (χ 2=14.7, P<0.001) and that was the only independent variable related to death in multivariate Cox proportional hazards analysis. By Kaplan-Meier analysis, there was no significant difference in deaths of patients with and without SA (χ 2=2.82, P=0.093). Over an average follow-up of 1,170☗63 days, 32 patients died. SA was noted in 58 patients (obstructive SA/central SA: 29/29). Averaged percutaneous oxygen saturation (SpO 2) during sleep was measured and an apnea-hypopnea index >5 was defined as SA. They underwent right-heart catheterization and a sleep study with simplified polysomnography. They were all in the Nice Classification group 1 (idiopathic PAH/associated PAH=52/48%, mean PAP of 46☑6 mmHg). Methods and Results: We enrolled 151 patients with PAH (44☑6 years old, male/female=37/114). 
The presence of SA is associated with a poor prognosis in patients with chronic left-sided heart failure, but little is known for patients with pulmonary arterial hypertension (PAH). Sleep apnea (SA) can cause repeated nocturnal arterial oxygen desaturation and result in acute increase in pulmonary arterial pressure (PAP).
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
